Baseline characteristics in the study population
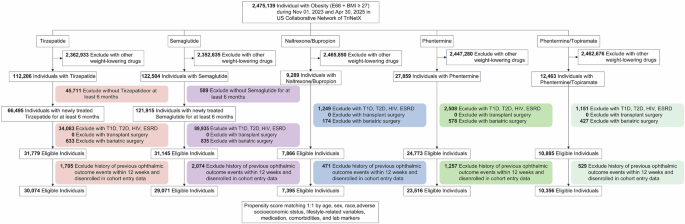
This analysis compared five anti-obesity medications, examining demographic characteristics, comorbidities, medication use, and laboratory markers before and after PSM (Supplementary Fig. 1). Initial cohorts exhibited substantial imbalances across treatment groups, with the Tirzepatide vs. Semaglutide comparison including 30,074 and 29,071 individuals, respectively, before matching (Supplementary Data 4). Mean age showed modest differences (47.3 ± 12.6 vs. 46.8 ± 14.6 years, SMD = 0.038), while more substantial disparities existed in racial distribution, with white individuals comprising 74.4% vs. 68.4% (SMD = 0.132). PSM substantially improved the balance between groups. The matched cohorts comprised 25,060 patients each, achieving excellent equilibrium across most variables. Age differences became negligible (47.5 ± 13.0 vs. 47.5 ± 13.2 years, SMD = 0.004), and racial distribution achieved balance (white: 72.6% vs. 72.3%, SMD = 0.006). Clinical conditions showed improved matching, with hypertensive disease prevalence (45.7% vs. 45.8%, SMD = 0.001) and most comorbidities reaching optimal balance.
The mean follow-up periods after matching; these durations remained relatively stable, with means ranging from 376.04 to 422.37 days, depending on the specific treatment comparison. The Tirzepatide groups consistently showed shorter mean follow-up periods (390.09–395.18 days), which corresponds to its more recent market introduction compared to the other medications studied (Supplementary Table 1).
Differential ocular outcomes: tirzepatide and semaglutide versus traditional anti-obesity medications
Our calendar-aligned analysis examining the period when all medications were simultaneously available in the market revealed several notable patterns in ocular outcomes (Figs. 2, 3, Supplementary Fig. 2, Table 1, and Supplementary Tables 2–7). Tirzepatide was associated with a significantly lower incidence of cataract development compared to Naltrexone/Bupropion (HR 0.46; 95% CI: 0.23–0.92; p = 0.025). When compared to Phentermine/Topiramate, Tirzepatide showed a lower cataract incidence (HR 0.76; 95% CI: 0.38–1.52; p = 0.433), though this did not reach statistical significance. Tirzepatide also demonstrated significant associations with reduced incidence of oculomotor binocular dysfunction compared to Naltrexone/Bupropion (HR 0.31; 95% CI: 0.16–0.60; p = 2.0 × 10−4), Phentermine (HR 0.44; 95% CI: 0.28–0.67; p = 1.0 × 10−4), visual issues and blindness versus Naltrexone/Bupropion (HR 0.44; 95% CI: 0.26–0.76; p = 0.003) and phentermine (HR 0.51; 95% CI: 0.35–0.74; p = 3.0 × 10−4), and visual disturbances against Naltrexone/Bupropion (HR 0.46; 95% CI: 0.26–0.83; p = 8.0 × 10−3) and Phentermine (HR 0.45; 95% CI: 0.31–0.68; p = 5.0 × 10−5; Fig. 2).

Statistical significance thresholds are indicated by horizontal reference lines on the negative log10 scale. The solid line represents the conventional exploratory significance level (−log10[0.05] = 1.30), while the dashed line denotes the Bonferroni-corrected threshold within each drug comparison (−log10[0.0083] = 2.08). The Bonferroni adjustment was applied to account for multiple testing across the six primary ocular outcomes, resulting in a revised significance threshold of 0.0083 (α = 0.05/6). Outcomes plotted above the dashed line meet the more stringent multiple comparison-adjusted criterion, whereas those between the solid and dashed lines achieve nominal statistical significance but require cautious interpretation in the context of multiple hypothesis testing.

Forest plot shows hazard ratios with 95% confidence intervals for ocular outcomes comparing anti-obesity medications in individuals with BMI ≥ 27 kg/m² (November 2023–April 2025). a presents Tirzepatide versus Semaglutide comparisons. b–g show comparisons against traditional medications: b Tirzepatide versus Naltrexone/Bupropion, c Phentermine, and d Phentermine/Topiramate; e Semaglutide versus Naltrexone/Bupropion, f Phentermine, and g Phentermine/Topiramate. Event counts appear below treatment names, with matched cohort percentages in parentheses. Horizontal error bars represent 95% confidence intervals from Cox proportional hazards models. Hazard ratios below 1.0 favor the first medication listed. Statistical testing used log-rank analysis with Bonferroni correction (p < 0.0083). NCOs negative control outcomes.
Semaglutide demonstrated lower cataract rates versus Naltrexone/Bupropion (HR 0.37; 95% CI: 0.18–0.75; p = 0.004), decreased oculomotor binocular dysfunction versus both Naltrexone/Bupropion (HR 0.46; 95% CI: 0.27–0.79; p = 0.004) and Phentermine (HR 0.42; 95% CI: 0.27–0.66; p = 1.0 × 10−4), and reduced visual disturbances versus Phentermine/Topiramate (HR 0.61; 95% CI: 0.38–0.97; p = 0.037) and Phentermine (HR 0.71; 95% CI: 0.51–0.98; p = 0.038; Fig. 2 and Supplementary Fig. 2).
In the Tirzepatide versus Semaglutide cohort of 25,060 matched pairs, no statistically significant differences emerged across ocular outcomes, though Tirzepatide showed a non-significant trend (HR 0.87, 95% CI: 0.55–1.37, p = 0.540; Fig. 3). When compared to Naltrexone/Bupropion, Tirzepatide demonstrated associations with lower incidence across multiple ocular outcomes. Cataract incidence was notably reduced (HR 0.46, 95% CI: 0.23–0.92, p = 0.025), representing a 54% lower observed rate. Similarly, oculomotor binocular dysfunction (HR 0.31, 95% CI: 0.16–0.60, p = 2 × 10−4), visual issues and blindness (HR 0.44, 95% CI: 0.26–0.76, p = 0.003), dry eye disease (HR 0.33, 95% CI: 0.15–0.71, p = 0.003), ametropic accommodative dysfunction (HR 0.31, 95% CI: 0.16–0.62, p = 2.3 × 10−4), and visual disturbances (HR 0.46, 95% CI: 0.26–0.83, p = 0.008) all showed statistically significant associations favoring Tirzepatide.
Against Phentermine/Topiramate, Tirzepatide demonstrated a significant association only with dry eye disease (HR 0.29, 95% CI: 0.15–0.57, p = 1.3 × 10−4), while other outcomes including cataracts (HR 0.76, 95% CI: 0.38–1.52, p = 0.433) and oculomotor binocular dysfunction (HR 0.63, 95% CI: 0.34–1.16, p = 0.134) showed non-significant trends. Compared to Phentermine alone, Tirzepatide showed significant associations with reduced oculomotor binocular dysfunction (HR 0.44, 95% CI: 0.28–0.67, p = 1.3 × 10−4), visual issues and blindness (HR 0.51, 95% CI: 0.35–0.74, p = 2.8 × 10−4), dry eye disease (HR 0.46, 95% CI: 0.27–0.79, p = 0.004), ametropic accommodative dysfunction (HR 0.44, 95% CI: 0.28–0.68, p = 1.9 × 10−4), and visual disturbances (HR 0.45, 95% CI: 0.31–0.68, p = 7 × 10−5).
Semaglutide comparisons with Naltrexone/Bupropion revealed significant associations with lower cataracts (HR 0.37, 95% CI: 0.18–0.75, p = 0.004), oculomotor binocular dysfunction (HR 0.46, 95% CI: 0.27–0.79, p = 0.004), dry eye disease (HR 0.36, 95% CI: 0.18–0.73, p = 0.003), and ametropic accommodative dysfunction (HR 0.50, 95% CI: 0.29–0.87, p = 0.012). Against Phentermine/Topiramate, Semaglutide showed significant associations with reduced dry eye disease (HR 0.26, 95% CI: 0.13–0.50, p = 2 × 10−5) and visual disturbances (HR 0.61, 95% CI: 0.38–0.97, p = 0.037). When compared to Phentermine, Semaglutide demonstrated significant associations with lower oculomotor binocular dysfunction (HR 0.42, 95% CI: 0.27–0.66, p = 1 × 10−4), dry eye disease (HR 0.61, 95% CI: 0.38–0.99, p = 0.044), ametropic accommodative dysfunction (HR 0.44, 95% CI: 0.28–0.70, p = 3.1 × 10−4), and visual disturbances (HR 0.71, 95% CI: 0.51–0.98, p = 0.038), while cataracts (HR 0.56, 95% CI: 0.31–1.00, p = 0.047) and visual issues and blindness (HR 0.77, 95% CI: 0.57–1.06, p = 0.105) showed borderline or non-significant associations.
The sensitivity analysis (individuals with BMI ≥ 30 kg/m2) generally reinforced findings from the BMI ≥ 27 kg/m2 population, with both GLP-1 RAs demonstrating consistent associations with better ocular outcomes compared to traditional anti-obesity medications (Fig. 3 and Supplementary Fig. 2).
Kaplan–Meier curves
The survival analysis approach through Kaplan–Meier estimation demonstrated distinct patterns in ocular health outcomes across different anti-obesity treatments (Supplementary Figs. 3–9).
Tirzepatide showed an observed association with lower incidence rates across multiple ocular conditions. When compared to Naltrexone/Bupropion combinations, the survival curves showed sustained separation throughout the observation period, with the most pronounced associations observed for oculomotor binocular dysfunction (HR 0.31, 95% CI: 0.16–0.60, p = 2.3 × 10−4), cataracts (HR 0.46, 95% CI: 0.23–0.92, p = 0.025), visual issues and blindness (HR 0.44, 95% CI: 0.26–0.76, p = 0.003), dry eye disease (HR 0.33, 95% CI: 0.15–0.71, p = 0.003), ametropic accommodative dysfunction (HR 0.31, 95% CI: 0.16–0.62, p = 4.3 × 10−4), and visual disturbances (HR 0.46, 95% CI: 0.26–0.83, p = 0.008). The temporal progression remained stable, indicating consistent associations rather than early transient effects. Compared to Phentermine/Topiramate, Tirzepatide showed an observed association with reduced incidence only for dry eye disease (HR 0.29, 95% CI: 0.15–0.57, p = 1.3 × 10−4), with other outcomes showing non-significant trends, including cataracts (HR 0.76, 95% CI: 0.38–1.52, p = 0.433).
Semaglutide was associated with a lower incidence across multiple comparisons. Against Naltrexone/Bupropion, observed associations with reduced incidence emerged for cataracts (HR 0.37, 95% CI: 0.18–0.75, p = 0.004), oculomotor binocular dysfunction (HR 0.46, 95% CI: 0.27–0.79, p = 0.004), dry eye disease (HR 0.36, 95% CI: 0.18–0.73, p = 0.003), and ametropic accommodative dysfunction (HR 0.50, 95% CI: 0.29–0.87, p = 0.012).
When compared to Phentermine/Topiramate, Semaglutide showed observed associations with lower incidence for dry eye disease (HR 0.26, 95% CI: 0.13–0.50, p = 2 × 10−5) and visual disturbances (HR 0.61, 95% CI: 0.38–0.97, p = 0.037).
Subgroup analysis
Based on the supplemental subgroup analyses, several notable patterns emerged regarding the associations between Tirzepatide and Semaglutide vs traditional anti-obesity medications across different patient characteristics and clinical contexts (Supplementary Data 5–22).
Among individuals with preserved renal function (eGFR ≥45 mL/min/1.73 m2), Tirzepatide demonstrated associations with reduced visual issues and blindness (HR 0.62, 95% CI 0.44–0.89) and visual disturbances (HR 0.58, 95% CI 0.39–0.86) compared to semaglutide. Among individuals without heart failure, Tirzepatide showed associations with reduced visual issues and blindness (HR 0.56, 95% CI 0.39–0.81) and visual disturbances (HR 0.52, 95% CI 0.35–0.78) compared to Semaglutide.
For Naltrexone/Bupropion comparisons, Tirzepatide showed associations with reduced cataract incidence, particularly in individuals without prior GLP-1 RA exposure (HR 0.18, 95% CI 0.05–0.60) and those without proteinuria (HR 0.34, 95% CI 0.13–0.85). Against Phentermine, Tirzepatide demonstrated associations with reduced oculomotor binocular dysfunction across most subgroups, with particularly strong associations in individuals with preserved renal function (HR 0.60, 95% CI 0.34–1.03) and those without ischemic heart disease (HR 0.55, 95% CI 0.30–0.98).
Semaglutide comparisons with traditional anti-obesity medications showed similar patterns. Against Naltrexone/Bupropion, Semaglutide demonstrated associations with reduced oculomotor binocular dysfunction, particularly in individuals with preserved renal function (HR 0.22, 95% CI 0.08–0.60) and those without prior GLP-1 RA exposure (HR 0.19, 95% CI 0.06–0.56).
Weight and HbA1c changes
Weight loss trajectories differed across medications (Supplementary Figs. 10 and 11). Tirzepatide produced 8.1% weight reduction from baseline (T-test, p = 9 × 10−4), exceeding Semaglutide’s 6.0% decrease (T-test, p = 2.45 × 10−8). Similarly, HbA1c reductions favored Tirzepatide at 5.1% versus Semaglutide’s 3.9% (T-test, p = 1.94 × 10−9; Supplementary Fig. 12).
Analysis of surgical interventions
To assess whether observed differences in cataract diagnosis translated into measurable healthcare utilization, we examined cataract surgery rates across treatment groups using CPT procedure codes (Supplementary Fig. 13). Surgical intervention rates remained comparable between Tirzepatide and Semaglutide (HR 1.92, 95% CI 0.63–5.87, p = 0.25). Tirzepatide showed no significant differences in surgery rates when compared with other agents: Naltrexone/Bupropion (HR 0.81, 95% CI 0.63–1.05, p = 0.11), Phentermine/Topiramate (HR 0.43, 95% CI 0.08–2.23, p = 0.30), or Phentermine (HR 3.21, 95% CI 0.61–16.91, p = 0.15).
Among Semaglutide comparisons, surgical rates showed no significant differences between Phentermine/Topiramate (HR 0.18, 95% CI 0.02–1.55, p = 0.08). Comparisons with Naltrexone/Bupropion (HR 0.55, 95% CI 0.16–1.95, p = 0.35) and Phentermine (HR 1.87, 95% CI 0.34–10.23, p = 0.46) showed no significant differences.
BMI-stratified analysis: medication-specific ocular protection patterns
The BMI-stratified subgroup analysis revealed no statistically significant differences between Tirzepatide and Semaglutide across primary ocular outcomes (Supplementary Fig. 14 and Supplementary Data 5–22). However, several statistically significant associations emerged when comparing these agents against traditional anti-obesity medications across different BMI categories.
Against Naltrexone/Bupropion, Tirzepatide demonstrated significant protective associations in specific BMI strata. For visual issues and blindness, the BMI 30–34.9 kg/m² group showed notable protection (HR 0.20, 95% CI 0.06–0.67). Visual disturbances outcomes favored Tirzepatide in the BMI 30–34.9 kg/m² category (HR 0.21, 95% CI 0.06–0.72). For visual disturbances, the BMI 30–34.9 kg/m² group demonstrated protective effects (HR 0.21, 95% CI 0.06–0.72). Against Naltrexone/Bupropion, Semaglutide exhibited significant protective associations in the BMI 30–34.9 kg/m² group for cataracts (HR 0.11, 95% CI 0.01–0.87). The comparison with Phentermine revealed significant protective associations for oculomotor binocular dysfunction in the BMI 27–29.9 kg/m² group (HR 0.12, 95% CI 0.01–0.93). Against Phentermine/Topiramate, Semaglutide demonstrated significant protection for dry eye disease in the BMI 35–39.9 kg/m² group (HR 0.18, 95% CI 0.04–0.83), representing a protective association in this specific weight category.
link






More Stories
Weight-Loss Drug Linked to Lower Risk of Eye Disease in Patients with Diabetes | Newsroom
Virtual reality exam checks eye health and screens for early signs of Alzheimer’s
Blindness and vision impairment