Characteristics of participants
The main characteristics of the participants are summarised in Table 1. The sample predominantly consisted of highly educated women, with 59.4% possessing undergraduate degrees, and healthcare professionals, accounting for 43.8%. The majority resided in urban areas (75%), with a mean age of 34.1 years.
Description of the GDM patient journey
The patient journey of individuals with gestational diabetes was analysed in three stages, focusing on 21 subcategories across three dimensions: health management tasks, emotions, and pain points. The experiences, challenges, and emotional changes of participants during health management were visualised, and their journey across stages and dimensions was systematically mapped (Fig. 3). To enhance conceptual clarity and analytical transparency, Table 2 presents the categories and subcategories identified through content analysis.
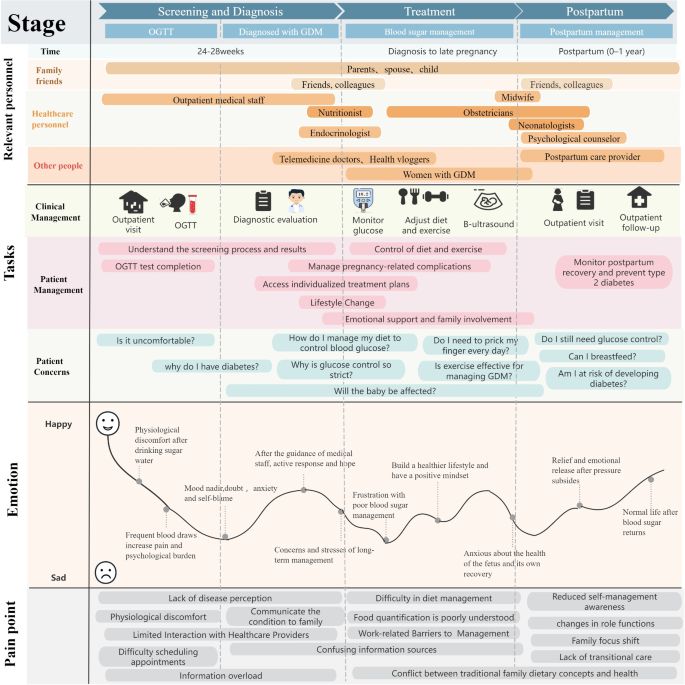
Patient journey mapping in gestational diabetes management
Screening and diagnostic stage
Tasks
Understanding and adhering to screening procedure
Patients needed to clearly understand the rationale and the strict requirements of the screening process, including fasting, timing, and repeated blood glucose tests. This understanding was essential to avoid errors (e.g., eating during the test, missing steps) that could invalidate results.
We have to do it once on an empty stomach, then once every hour, and then twice every two hours. It takes a long time. For standard tests, you must check three times, one of which is high, indicating diabetes; therefore, you must check it thoroughly (Participant 5)..
Engaging in treatment plan decision-making
After diagnosis, women’s task was not only to get professional advice but also to decide how to incorporate it into their daily routines. This often meant visiting nutrition clinics and adjusting their diet based on individual recommendations.
I didn’t know what to do next, so I followed my obstetrician’s advice and went to the nutrition clinic. She said she might be able to help me adjust my diet (Participant 4).
Developing awareness of disease seriousness
Participants must understand the seriousness of gestational diabetes and its potential health risks for both mother and fetus. Gaining a clear understanding of the disease’s importance helps pregnant women see that an accurate diagnosis is not just a routine medical step, but a vital measure to protect maternal and fetal health.
I must fast according to hospital regulations and arrive on time for the test, as I understand that failing to meet the test requirements could lead to inaccurate results, which would jeopardize the health of both myself and my baby (Participant 7).
Emotional responses to diagnosis
Initial psychological resistance
When diagnosed with GDM, participants often initially resist psychologically, showing signs like shock, confusion, or denial. This reaction was especially common among those who saw themselves as healthy, had no previous symptoms, or didn’t think they were at risk. Participants frequently doubted the accuracy of the diagnosis or minimized its seriousness.
I didn’t understand how I could have it. I don’t even like sweets (Participant 8).
I was shocked because everything was normal before 24 weeks, and I did not expect to have diabetes (Participant 14).
Pain points
Physical and procedural burdens
Participants described the OGTT as especially difficult, mentioning both the physical discomfort of drinking a concentrated glucose solution on an empty stomach and the hassle of repeated blood draws and long hospital stays. These combined factors made the test stressful and tiring, with several women describing it as a major source of pressure during the screening phase.
The diagnostic process of drinking sugar water is challenging, not just for me but for many pregnant women in the clinic. Some even vomited shortly after drinking it. The sugar water is hard to swallow; it is super sweet and overwhelming. Moreover, drinking such a high-concentration sugar water on an empty stomach is quite uncomfortable (Participant 18).
The frequent blood tests made the process feel overwhelming and forced me to spend much longer in the hospital than I expected (Participant 21).
Insufficient early education and disease awareness
Most participants reported entering the screening and diagnostic stage with little or no prior knowledge of GDM. This “cognitive gap” was mainly linked to the lack of systematic early education and limited public health promotion. Consequently, women’s understanding of GDM often depended almost entirely on information given during their first antenatal visit.
I feel that the publicity efforts are still insufficient, because you rarely see any promotion about GDM. You only come across relevant educational content when you visit the obstetrics clinic or maternity ward (Participant 15).
I am unsure what kind of illness this is because we do not have it in our family, and I do not know anyone around me who has it, so I do not know what it is (Participant 25).
Treatment stage
Health management tasks
Lifestyle-based blood glucose management
Participants mainly relied on lifestyle changes, especially diet and exercise, to control their blood sugar levels. Following recommended meal plans, avoiding foods high in sugar or fat, and engaging in moderate physical activity were common approaches. Many participants described organizing their daily routines around these habits, emphasizing the importance of consistency in keeping blood glucose stable.
I avoid sweets and fried foods and always take a short walk after lunch and dinner. It’s tiring at times, but I know it helps control my blood sugar (Participant 7).
I follow my doctor’s advice on controlling my diet, avoiding fruit as much as possible, and taking a walk after every meal. This has helped me keep my blood sugar levels well under control. (Participant 20).
Understanding blood glucose patterns
Participants highlighted the importance of not only tracking blood glucose but also identifying patterns in their readings and understanding factors that cause fluctuations. This knowledge helped them make better choices about diet, activity, and medication, boosting their confidence in self-management.
I started noticing my blood sugar was higher in the morning or after certain foods. Knowing this helped me adjust my diet and exercise” (Participant 9).
Tracking my readings over several days showed me which habits worked and which didn’t. It gave me more control (Participant 14).
Family involvement in self-management
Participants emphasized the importance of family in supporting blood glucose management by offering oversight and aligning household routines with medical recommendations. Active family involvement improved adherence to lifestyle changes and fostered a shared understanding of disease management.
Involving my parents during doctor visits helped them understand what I need to do, so they can support me at home(Participant 11).
When my husband follows the same diet guidelines, it’s much easier for me to stick to my plan (Participant 22).
Emotions
Distress and anxiety over loss of control
When blood glucose levels improve, participants feel a sense of accomplishment and psychological relief, which confirms the effectiveness of their efforts, boosts their self-efficacy, and reinforces their confidence in maintaining a healthy lifestyle.
Sometimes, even though I’ve been strict with my diet, my blood sugar is still high and hard to control. I’m worried that if I can’t control my blood sugar well, it might affect the health of my baby (Participant 30).
Validation and enhanced self-efficacy
When blood glucose levels improve, participants feel a sense of accomplishment and psychological relief, which affirms the effectiveness of their efforts, boosts their self-efficacy, and reinforces their confidence in maintaining a healthy lifestyle.
When my blood sugar levels aren’t as high, it feels like all my efforts are paying off, making me happy. It gives me hope that I can have a healthier lifestyle (Participant 31).
Pain points
Challenges in dietary adherence
Participants especially struggled with dietary management, finding it difficult to strictly follow dietary restrictions daily and facing challenges with food choices, portion sizes, and practical implementation.
If you’re trying to measure everything down to the exact grams, it’s hard to do that in a regular household when cooking (Participant 2).
The hardest part after getting pregnant is wanting to eat certain things but not daring to, because controlling my diet feels so difficult (Participant 27).
Contextual barriers to blood glucose management
Pregnant women often face time constraints, environmental limitations, and social pressures in their work or daily life, making it difficult to eat at regular intervals or maintain stable blood glucose levels.
For those of us working during pregnancy, it’s challenging to have snacks in between meals. If we do manage to snack, it’s usually just something like fruit (Participant 2).
Because this disease is straightforward, I may be embarrassed to say that I am often hungry, which makes me feel a little hypocritical (Participant 18).
Digital support for self-management
Participants hope to use technological tools, such as apps or digital platforms, to conveniently record their blood glucose levels and dietary intake, receive real-time analysis and personalized guidance, and reduce the need for in-person medical visits.
It would be great to have a dedicated app that monitors blood sugar levels daily…so you don’t have to go to the doctor every time you measure your blood sugar (Participant 15).
Postpartum stage
Tasks
Continuous blood glucose monitoring
Participants continued to monitor their blood glucose after childbirth due to concerns about developing diabetes. Sustained self-monitoring was seen as essential for early detection and prevention of complications.
After giving birth, I continue to check my blood sugar regularly to keep track of my health and reduce the risk of developing diabetes (Participant 18).
Postpartum lifestyle maintenance
Some participants successfully integrated the dietary and exercise habits they adopted during pregnancy into a proactive, sustainable approach to managing their health. Even after reaching normal blood glucose levels postpartum, they intentionally limited sugar intake and kept exercising, marking a shift from externally directed management to self-motivated self-care.
During pregnancy, I learned to control my fruit intake and keep active. Even after giving birth, I still try to limit sugar and engage in regular exercise to maintain my health (Participant 7).
Managing maternal-infant health balance
Participants faced the challenge of balancing their own health management with newborn care. Task conflicts arose when caregiving responsibilities limited the time available for self-care, highlighting the need for strategies that support both maternal and infant well-being.
After my baby was born, I had to think about both my own health and the baby’s. I try to eat carefully and check my blood sugar when I can, but I have to plan around taking care of the baby (Participant 13).
Emotions
Anxiety about future health
After childbirth, participants experienced anxiety related to potential long-term risks of impaired insulin function or developing type 2 diabetes. This concern was compounded by the physical and psychological stress of postpartum recovery, including sleep deprivation and reduced opportunity for exercise.
I was concerned after giving birth, because some people often say that if this disease is not well managed, it will turn into diabetes (Participant 13).
Pain points
Decreased attention to self-management
After postpartum blood glucose levels return to normal, many participants experience a rapid decline in their perceived long-term risk of GDM. Without clear abnormal results as a warning signal, their “patient” identity loses salience, leading to decreased attentiveness in self-management and a diminished sense of urgency to maintain a healthy lifestyle
“After giving birth, I had my blood sugar tested once and it was normal, so I stopped paying attention to it (Participant 18).
Maternal role and self-care conflict
Postpartum participants face a conflict between caregiving and self-health management. Newborn care demands often lead to deprioritization or interruption of health tasks, while family focus shifts from maternal well-being to infant development.
Instead, we only focus on whether the child’s development indicators meet the standard. Ordinary families don’t pay much attention to the mother’s situation anymore (Participant 2).
After the baby was born, I had no time to think about myself. I stopped checking my blood sugar—I was too tired (Participant 6).
Cultural and dietary challenges
Postpartum women often face a conflict between traditional “confinement” diets and modern medical nutrition advice. Family-endorsed high-calorie diets to support lactation can destabilize blood glucose, while women worry that restrictions may affect milk supply. These cultural beliefs and family pressures make it difficult to follow individualized nutrition plans.
I didn’t know how to eat it at first, it would be suitable for the milk, and I wouldn’t overgrow, which was after my first child. I have a distorted perspective, and my family does not recognise this aspect of the situation, namely, that the intake exceeds the need. Consequently, I gained 10 pounds during the confinement period, and the amount of milk was not substantial (Participant 17).
link






More Stories
Beyond Morning Sickness: Hyperemesis Gravidarum
NEWS: ICE has been deporting pregnant and postpartum immigrants
How much exercise is safe during pregnancy? New research offers answers